Breast cancer is the most common type of cancer in women. In Spain, nearly 30% of cancers diagnosed originate in the breast. Although its incidence has grown in recent years, advances in treatment and early diagnosis of the disease deliver an increasingly improved prognosis.
Tomas Arrazola, a pharmacist specialising in oncological pharmacy at HC Marbella and HC Ceuta, talks about the new drugs currently being given to treat this disease.
How have breast cancer drugs evolved?
Fortunately, in recent years knowledge of the molecular biology of tumours has increased, allowing the development of treatments which improve on the results from classic chemotherapy. They are basically of two types, the first are treatments which target specific mutations and the second are immunotherapy drugs which bolster our immune system so it recognises and attacks the tumour.
What new drugs are there?
Before we discuss new drugs for breast cancer, we need to have some understanding of the 3 breast cancer subtypes: luminal, HER2 and triple negative. The novel approaches to treatment are based on this information.
Luminal: this subtype of breast cancer is highly hormone dependent and is treated with drugs which block the action of these hormones. Cell cycle inhibitors such as Ribociclib, Palbociclib and Abemaciclib used in advanced disease are no longer new drugs, and there is growing evidence that they may be useful neoadjuvant and adjuvant treatments in localised disease. When these drugs are used in advanced disease, at some point they lose their effect; 50% of the time this loss of effect is due to a PIK3CA mutation for which we have a drug called Alpelisib. This drug is not yet available commercially, but we have treated 5 patients with it in our centre with encouraging results.
HER2: This subtype is characterised by its HER2 receptor amplification and is the most aggressive, however, the arrival of Trastuzumab in early 2000 resulted in a radical change in both the treatment and prognosis of the disease. Trastuzumab results have been improved further by the introduction of Pertuzumab, in combination with Trastuzumab, in both advanced and localised disease. Subsequently antibody-drug conjugates arrived, these combine a monoclonal antibody with a cytotoxic drug with the aim of targeting the cytotoxic drug at the cell that has the HER2-amplified receptor, thus destroying it. Unlike when receiving conventional chemotherapy, other healthy cells are largely prevented from being affected. These antibody-drug conjugates use Trastuzumab as a shuttle, they are Trastuzumab-Emtansine and Trastuzumab-Deruxtecan, the latter has delivered results never seen before in the heavily pre-treated patients treated in our centre. Trastuzumab-Deruxtecan has recently delivered impressive data even in those patients who have breast cancer with weak HER2 expression.
Triple negative: the name as such lacks definition, it has no hormone receptors for oestrogen or progestogen, or amplification of the HER2 receptor, it is the most aggressive form and there are fewer drug treatments available. Fortunately, there is a ray of hope as these are highly immunogenic tumours in which immunotherapy drugs can play a key role. Both Atezolizumab and now Pembrolizumab have been approved by regulatory agencies for their use in advanced disease; data also exists on localised disease, with Pembrolizumab indicated as neoadjuvant treatment and as adjuvant treatment afterwards.
Within this subtype, not an insignificant percentage of patients have a BRCA gene mutation which contributes to an error in DNA repair. These patients are candidates for treatment with Olaparib or Talazoparib in advanced disease, or even Olaparib as adjuvant treatment in the case of localised disease.
Triple-negative conjugated antibodies such as Sacituzumab-Govitecan are also now available, already approved in the USA, they will be available in Europe in the near future.
At HC, we are committed to innovative treatment and to providing the latest alternative drug treatments for our patients, even if they are not yet generally available. We are increasing the range of new emerging treatments through involvement in new clinical drug trials.
Breast Cancer Screening
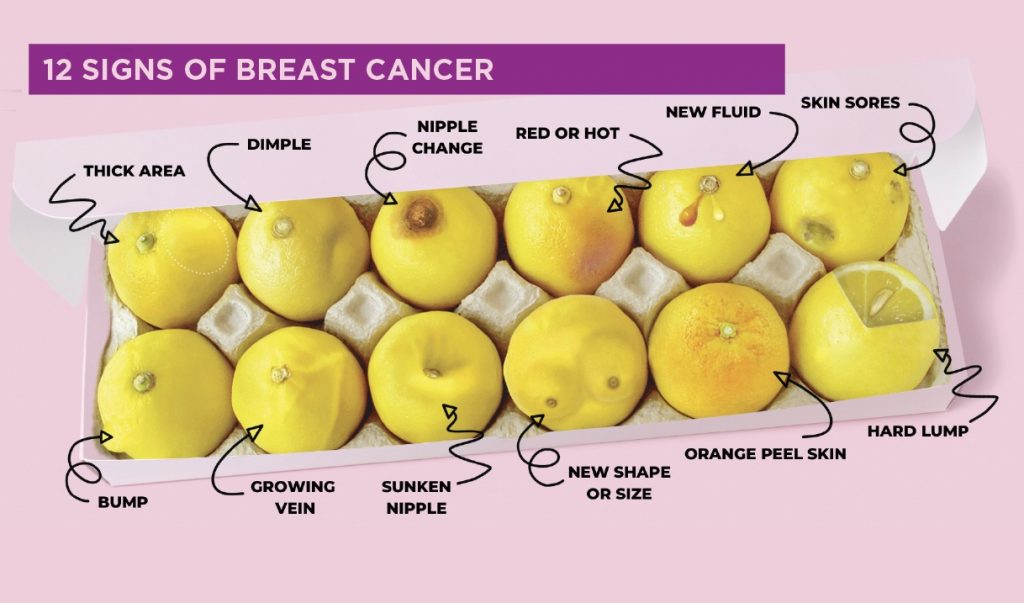
October marks breast cancer awareness month, and awareness of breast cancer is crucial to early detection and better health outcomes. In some cases it will be possible to notice visible changes to the breast, check out the ‘Know Your Lemons’ website and app for more details. However breast screening is the best tool we currently have to help detect cancers before there are signs of disease, when for example they are too small to feel.
In Gibraltar, women between the ages 40 and 70 are invited for screening mammograms at 2-yearly intervals.
Trans men, trans women and anyone non-binary (between 40 – 70 years) may be invited automatically or may need to talk to the local breast screening team.
Anyone can get breast cancer.
This includes women, men, trans and non-binary people.
•
The chance of getting breast cancer increases as you get older.
•
Most breast cancers are diagnosed in women over 50 years old.
It is important for all those who are eligible to take advantage of the screening program. Invitations are sent in the form of a slip which must be returned to the screening nurses in order to obtain an appointment.
You can have breast screening whatever size or shape your breasts are. Those with implants can also be screened safely; there are several methods mammographers (specialists who help take the breast x-rays) use.
Breast screening cannot stop someone getting breast cancer, but it is the best way to spot cancers at an early stage.
Finding cancers early can make it:
•
more likely that treatment will be successful
•
less likely you’ll need to have any surgery
• more likely you’ll be cured
If you are eligible for screening and have not been contacted, or wish to make an appointment or just find out more, contact:
GHA Breast Screening Team
Call : 200 72266 Ext.2214
Email: BreastScreening@gha.gi